Abstract
Background Although severe dementia could protect against suicide death by decreasing a person’s capacity to implement a suicide plan, patients with early dementia may have better cognition, giving them more sustained insight into their disease and better enabling them to carry out a suicide plan. This study investigated suicide risk in older adults within 1 year of receiving a diagnosis of dementia.
Methods This study used National Health Insurance Service Senior Cohort data and included 36 541 older adults with newly diagnosed dementia (a Mini-Mental State Examination score ≤ 26 and a Clinical Dementia Rating score ≥ 1 or a Global Deterioration Scale score ≥ 3), including Alzheimer disease, vascular dementia and other/unspecified dementia, from 2004 to 2012. We selected older adults without dementia through 1:1 propensity-score matching using sex, age, comorbidities and index year, with follow-up throughout 2013. We estimated adjusted hazard ratios (AHRs) of suicide deaths within 1 year after diagnosis using a time-dependent Cox proportional hazards model.
Results We verified 46 suicide deaths during the first year after a dementia diagnosis. Older adults with dementia had an increased risk of suicide death compared to those without dementia (AHR 2.57; 95% confidence interval [CI] 1.49–4.44). Older adults with Alzheimer disease (AHR 2.50; 95% CI 1.41–4.44) or other/unspecified dementia (AHR 4.32; 95% CI 2.04–9.15) had an increased risk of suicide death compared to those without dementia. Patients with dementia but without other mental disorders (AHR 1.96; 95% CI 1.02–3.77) and patients with dementia and other mental disorders (AHR 3.22; 95% CI 1.78–5.83) had an increased risk of suicide death compared to patients without dementia. Patients with dementia and schizophrenia (AHR 8.73; 95% CI 2.57–29.71), mood disorders (AHR 2.84; 95% CI 1.23–6.53) or anxiety or somatoform disorders (AHR 3.53; 95% CI 1.73–7.21), respectively, had an increased risk of suicide death compared to patients with those conditions but without dementia.
Limitations This study examined only elderly patients in South Korea, a population with a substantially higher suicide rate than the global population. Caution must be exercised when generalizing the results to populations with dissimilar backgrounds.
Conclusion Patients with dementia had an increased risk of suicide death within 1 year after diagnosis compared to those without dementia.
Introduction
Suicide is one of the most important public health issues affecting older adults.1,2 Although in most countries suicide attempts are more frequent among young people, the mortality rate of suicide is higher among older adults.3,4 In 2016, South Korea was ranked tenth globally according to suicide rate (20.2 per 100 000 people); the rate among older adults (age ≥ 60 years) in the same year was 53.3 per 100 000 population, the highest of all countries in the Organisation for Economic Co-operation and Development.5,6 Considering the rapid growth in the elderly population in South Korea (mean 4.1% annually) and the country’s higher proportion of the elderly in the total population (14.3% in 2018) compared to the global population (8.2%),7 there is a need for continued research into the causes of suicide among older adults in South Korea.
Dementia is one of the major health care problems in later life, affecting 24 million people worldwide.8 A review of global figures on dementia reported an age-standardized prevalence for people older than 60 years of 5% to 7%,9 and the occurrence of suicidal ideation in an older person with dementia varied from 6% to 24%.10 Although high rates of psychiatric symptoms in dementia have been reported,11 the risk of suicide in people with dementia has received relatively little attention; suicidal behaviour in these people is generally not regarded as likely12 because of cognitive limitations,13,14 restricted access to a means of suicide and the reduced possibility of planning a suicidal act because of increased surveillance.15
However, specific features of dementia might increase the risk of suicide. Behavioural and psychological symptoms of dementia (also known as neuropsychiatric symptoms of dementia) are core features.16 Behavioural and psychological symptoms affect up to 90% of patients with dementia at some time during their illness.17 Patients with these symptoms experience emotional distress, diminished quality of life, greater functional impairment, more frequent hospitalizations and increased risk of abuse and neglect.18 A previous study reported that patients with dementia and suicidal ideation had a significantly higher rate of behavioural and psychological symptoms.19 Patients with dementia affected by behavioural and psychological symptoms may demonstrate an increased risk of suicide.
Compared to data on suicide risk in people without dementia, data in people with dementia are scarce and based primarily on case reports20–22 or studies of risk factors for suicide among people with dementia.10,19,23–27 Two studies have examined suicide risk in patients with dementia compared to those without dementia.28,29 However, these studies included patients diagnosed with dementia during full-time admission to somatic or psychiatric hospitals28 or patients with dementia who died by suicide and who were in contact with mental health services.29 Therefore, data on suicide risk remain limited in patients who have dementia but not other mental disorders. Furthermore, mental disorders are major risk factors for suicide,30 but previous studies have not assessed suicide risk according to diagnostic timing or subcategories of other mental disorders in patients with dementia.
Severe dementia could protect against suicide death by decreasing a person’s capacity to implement a suicide plan.31 In contrast, patients with early dementia may have better cognition, giving them more sustained insight into their disease and better enabling them to carry out a suicide plan.12 We hypothesized that the period within 1 year of a dementia diagnosis would be associated with higher suicide risk. Previous studies have reported that suicide risk is highest within 1 year after diagnosis of diseases such as cancer and stroke;32–36 information about suicide risk in the 1 year after dementia diagnosis is unavailable.
We examined suicide deaths during the first year after a dementia diagnosis (Alzheimer disease, vascular dementia or other dementia) in older adults. We identified suicide risk based on the diagnostic timing of other mental disorders. We analyzed variations in suicide risk by subcategories of mental disorders (substance use disorders, schizophrenia, mood disorders, anxiety and somatoform disorders, and other mental disorders). We also explored suicide risk in older adults with dementia according to sex, age and comorbidities.
Methods
Data and study sample
This study used National Health Insurance Service–Senior Cohort data supplied by the Korean National Health Insurance Service. The National Health Insurance Service data covered a 10% random sample of the elderly population aged 60 years or older (5.5 million people) in 2002. Unless disqualified because of emigration or death, participants were followed up for 12 years, until 2013. Information for each person’s cause of death was extracted from Statistics Korea and linked with our database. The National Health Insurance Service–Senior Cohort data include demographics and clinical information about diagnoses, treatments and prescribed drugs for all medical institution visits, such as clinics, hospitals and pharmacies.
Of the 528 655 people from the National Health Insurance Service–Senior Cohort between 2004 and 2012, we divided study participants into adults with dementia (n = 37 404) and adults without dementia (n = 491 251). We determined that a person had dementia if they were first prescribed an antidementia drug (donepezil, galantamine, rivastigmine or memantine) in association with International Classification of Diseases 10th Revision (ICD-10) codes F00–F03, F05.1, G30 or G31 from Jan. 1, 2004, to Dec. 31, 2012. Dementia was further classified as Alzheimer disease (ICD-10 codes F00 or G30), vascular dementia (ICD-10 code F01) or other/unspecified dementia (ICD-10 codes F02, F03, F05.1 or G31). According to relatively strict criteria, dementia was diagnosed based on evidence for cognitive dysfunction: a Mini-Mental State Examination score of 26 or less and a Clinical Dementia Rating score of 1 or more, or a Global Deterioration Scale score of 3 or more.37–39 Of those with dementia, we excluded people with dementia in 2002 and 2003 (n = 863) to include only those with newly diagnosed dementia.
For comparison, we selected elderly people without dementia (n = 491 251) from 2004 to 2012; people with dementia between 2002 and 2003 (n = 703) were excluded. To reduce selection bias, we conducted 1:1 propensity-score matching. The propensity-score matching technique consists of matching individuals in different groups who have propensity scores that are the same or similar.40 The propensity score was computed as the probability of being diagnosed with dementia using multivariable logistic regression in which sex, age, comorbidities and index year were included as covariates. People were divided into categories of young-old (age 60–74 years) and old-old (age > 75 years) based on a previous study.41,42 The year of the first diagnosis of dementia in the study period was defined as the index year, and the members of the comparison group were matched with patients with dementia in the same index year. The comorbidities were diabetes mellitus (ICD-10 codes E10–E14), hypertension (ICD-10 codes I10–I15), dyslipidemia (ICD-10 code E78), Parkinson disease (ICD-10 code G20), stroke (ICD-10 codes I60–I63), ischemic heart disease (ICD-10 codes I20–25), chronic kidney disease (ICD-10 code N18) and cancer (ICD-10 codes C00–C99) and were estimated by screening information from medical records before the index date. The index date was the date of each person’s first diagnosis. The matching process was performed using a greedy algorithm with a caliper of 0.2 times the standard deviation of the propensity scores. The greedy algorithm was used so that, once a match was made, it was not reconsidered.43 We evaluated covariate balance before and after matching using p values; the p values for matching variables (sex, age, comorbidities and index year) between patients with dementia and patients without dementia after matching were approximately 1.000, indicating that the characteristics of the matching variables between the 2 groups were the same. In the end, this study included patients with dementia (n = 36 541) and without dementia (n = 36 541; Appendix 1, Fig. S1, available at jpn.ca/190219-a1).
Measurements
Suicide death (ICD-10 codes X60–X84) within 1 year of the index date was the dependent variable. Survival duration was measured in days, and all patients were followed up from index dates until suicide death, withdrawal from the medical security system (National Health Insurance Service subscribers or Medical Aid beneficiaries), death from other causes or the end of 2013, whichever occurred first.
Potential confounding factors were residential area, household income, disability, insurance type and other mental disorders. Except for other mental disorders, information on these factors was based on the patient’s index year. Because the status of the potential confounding factors could change over time, we measured this information from the index date to the final date for each year during the study period (2004–2013). We used time-dependent covariates for age, household income, insurance type, residential area and disability. Household income was classified as low (< 40th percentile), middle (41st–80th percentile) or high (81st–100th percentile). Residential area was classified as metropolitan (capital), urban (local government where > 1 million people live) or rural (other areas). Insurance type was classified as National Health Insurance or Medical Aid, which is a public medical support policy that assists poor people. Disability was defined according to the term registered by the Korean government after a physician’s diagnosis for disability.44
We also considered other mental disorders as confounding factors in this study. We measured first diagnoses of other mental disorders using ICD-10 codes as a primary diagnosis. These were classified as substance abuse disorders (ICD-10 codes F10–F19), schizophrenia (ICD-10 codes F20–F29), mood disorders (ICD-10 codes F30–F39), anxiety and somatoform disorders (ICD-10 codes F40–F48) and other mental disorders (ICD-10 codes F49–F99). We also created 3 categories based on the onset of the other mental disorder(s): patients with dementia but without other mental disorders; patients diagnosed with other mental disorders before they were diagnosed with dementia (from Jan. 1, 2002); and patients who were diagnosed with other mental disorders after they were diagnosed with dementia. We did not use other mental disorders as a time covariate variable in this study because the absence of a diagnosis record for the year after a diagnosis of another mental disorder did not imply that patients were completely treated for their mental disorder.
Statistical analysis
We summarized patients’ baseline characteristics by dementia status. We tested the statistical significance of the proportional differences in characteristics between patients with dementia and the comparison group using the Pearson χ2 test. We presented average person-years from the index date to the date of the final event and the number of suicide deaths within 1 year after diagnosis per group. Based on person-years at risk and number of suicide deaths, we calculated the number of suicide deaths per 100 000 person-years. We used the time-dependent Cox proportional hazards model to evaluate suicide risk within 1 year after the index date. We reported the results as adjusted hazard ratio (AHR) estimates with 95% confidence intervals (CIs). Events other than suicide death within 1 year from the index date were censored in the survival analysis.
First, we estimated the AHR and 95% CI suicide risk for older adults with dementia compared to those without dementia. Next, we analyzed suicide risk for older adults with dementia by subtype of dementia (Alzheimer disease, vascular dementia or other/unspecified dementia) compared to those without dementia. Third, we estimated suicide risk for older adults with dementia by the presence of other mental disorders, by the diagnostic timing of other mental disorders and by subcategories of mental disorders (substance use disorders, schizophrenia, mood disorders, anxiety and somatoform disorders, and other mental disorders) compared to patients without dementia. Finally, we measured suicide risk for older adults with dementia according to sex, age group and comorbidities compared to those without dementia. We defined patients with comorbidities as those with 1 or more comorbidities. All data set extraction and statistical analyses were conducted using SAS 9.4 software; proportional hazards assumptions were evaluated statistically and satisfied for all models.
Results
Table 1 presents patients’ baseline characteristics between 2004 and 2012. Before propensity-score matching, all confounding factors between older adults with and without dementia were significantly different. After matching, 70.0% of patients were women, and 30.5% and 69.5% were in the young-old and old-old groups, respectively. Patients with dementia had histories of diabetes (60.6%), hypertension (81.3%), dyslipidemia (61.4%), Parkinson disease (8.2%), stroke (43.9%), ischemic heart disease (41.9%), chronic kidney disease (3.4%) and cancer (18.9%). The proportions of patients with histories of comorbidities were similar to those of the matched comparison group. The proportion of patients with a high household income was higher in older patients with dementia than in the matched comparison group (36.9% v. 35.6%, p < 0.001). The proportion of people receiving Medical Aid was higher in older adults with dementia than in the matched comparison group (14.2% v. 11.3%, p < 0.001). The proportion of older adults with dementia with a disability was higher than in the matched comparison group (1.9% v. 1.3%, p < 0.001). The proportion of those with other mental disorders was higher in older adults with dementia than in the matched comparison group (47.8% v. 35.5%, p < 0.001). There was no significant association between residential area and dementia (p = 0.64).
Study participants’ general characteristics (2004–2012)
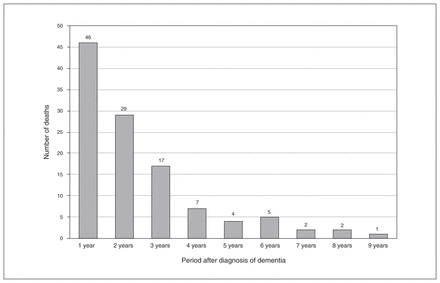
Figure 1 indicates the number of suicide deaths by period after dementia. Of the 36 541 patients with dementia, 113 died by suicide over the entire follow-up period. The median time from dementia diagnosis to suicide death was 1.22 years (range 0.01–8.18 years), and the number of suicide deaths decreased progressively with time after dementia diagnosis. In the first 9 years after a dementia diagnosis, 46 (40.9% of the total), 29, 17, 7, 4, 5, 2, 2 and 1 suicide occurred. Because the sizes of the populations followed per period after dementia diagnosis were different, we measured suicide rates per 100 000 person-years according to the period after dementia diagnosis. The suicide rate was the highest in the first year (125.9) and varied over the years that followed: second (88.4), third (72.6), fourth (44.1), fifth (39.5), sixth (83.7), seventh (54.8), eighth (100.1) and ninth (115.1).
Number of suicide deaths by period after diagnosis of dementia.
Table 2 shows suicide risk within 1 year after a diagnosis of dementia. Model 1 indicated that older adults with dementia were at higher risk of suicide death than the comparison group (AHR 2.57, 95% CI 1.49–4.44; p < 0.001). Model 2 shows that suicide risk was higher among older adults with Alzheimer disease (AHR 2.50, 95% CI 1.41–4.44; p = 0.002) and other/unspecified dementia (AHR 4.32, 95% CI 2.04–9.15; p< 0.001) than among those without dementia. However, vascular dementia (AHR 0.94, 95% CI 0.22–4.04; p = 0.93) was not significantly correlated with suicide risk.
Suicide risk within 1 year after dementia diagnosis
Table 3 shows suicide risk within 1 year after a diagnosis of dementia according to the presence and diagnostic timing of other mental disorders. In model 1, patients with dementia but without other mental disorders (AHR 1.96, 95% CI 1.02–3.77; p = 0.044) and patients with dementia and other mental disorders (AHR 3.22, 95% CI 1.78–5.83; p < 0.001) had an increased risk of suicide death compared to patients without dementia. In model 2, patients diagnosed with other mental disorders before dementia (AHR 3.77, 95% CI 2.05–6.91; p< 0.001) had an increased risk of suicide death compared to patients without dementia, whereas patients diagnosed with other mental disorders after dementia (AHR 1.46; 95% CI 0.43–4.97; p = 0.54) did not have an increased risk of suicide death compared to those without dementia.
Suicide risk within 1 year after dementia diagnosis by other mental disorders
Table 4 shows suicide risk within 1 year after dementia diagnosis according to subtypes of other mental disorders. Compared to patients without dementia, patients with dementia and schizophrenia (AHR 8.73, 95% CI 2.57–29.71; p < 0.001), mood disorders (AHR 2.84, 95% CI 1.23–6.53; p = 0.014) and anxiety and somatoform disorders (AHR 3.53, 95% CI 1.73–7.21; p < 0.001) had an increased risk of suicide death, whereas patients with dementia and substance use disorders (AHR 4.73, 95% CI 0.63–35.43; p = 0.13) and other mental disorders (AHR 1.83, 95% CI 0.54–6.23; p = 0.33) did not have an increased risk of suicide death.
Suicide risk within 1 year after dementia diagnosis by subtypes of other mental disorders
Table 5 indicates suicide risk within 1 year after dementia according to sex, age and comorbidities. Both men (AHR 2.50, 95% CI 1.19–5.23; p = 0.015) and women (AHR 2.75, 95% CI 1.22–6.19; p = 0.014) with dementia had an increased risk of suicide death compared to those without dementia. Both young-old adults with dementia (AHR 4.58, 95% CI 1.55–13.58; p = 0.006) and old-old adults with dementia (AHR 2.01, 95% CI 1.06–3.83; p = 0.033) had an increased risk of suicide death compared to those without dementia. Patients with dementia and comorbidities (AHR 3.17, 95% CI 1.74–5.79; p < 0.001) had an increased risk of suicide death compared to those without dementia. In contrast, patients with dementia and without comorbidities (AHR 0.49, 95% CI 0.09–2.68; p = 0.41) did not have an increased risk of suicide death compared to those without dementia.
Suicide risk within 1 year after dementia by sex, age and comorbidities
Discussion
We examined suicide risk within 1 year after dementia diagnosis (a Mini-Mental State Examination score of 26 or less and a Clinical Dementia Rating score of 1 or more, or a Global Deterioration Scale score of 3 or more) and generated 4 main findings. First, older adults with dementia had a higher risk of suicide death than older adults without dementia. Second, older adults with Alzheimer disease and other/unspecified dementia had a higher risk of suicide death than older adults without dementia. Third, patients with dementia with or without other mental disorders had a higher risk of suicide death than patients without dementia. In patients with other mental disorders, those diagnosed with the other mental disorders before they were diagnosed with dementia had an increased risk of suicide death. Patients with dementia and schizophrenia, mood disorders, or anxiety or somatoform disorders had an increased risk of suicide death. Finally, men and women with dementia, young-old and old-old adults with dementia, and patients with dementia and comorbidities all had an increased risk of suicide death compared to those without dementia.
A Danish study examined the risk of suicide in 21 394 people aged 50 years and older who were diagnosed with dementia during hospitalization from Jan. 1, 1990, to Dec. 31, 2000. Their results showed that older adults with dementia had an elevated risk of suicide compared to those without dementia.28 A survey in England and Wales included 11 512 people aged 10 years and older who died by suicide and were in contact with mental health services between April 1996 and December 2004. The study found that significantly fewer suicides occurred in patients with dementia than in those without dementia.29 The studies’ different results may be attributable to the characteristics of the study population. Our findings showed that older adults with dementia had an increased risk of suicide death within 1 year after diagnosis compared to patients without dementia. These findings suggest that the early period after diagnosis is important for predicting suicide risk in older adults with dementia. Furthermore, patients with dementia but without other mental disorders also had an increased risk of suicide death. Clinicians need to recognize that following a dementia diagnosis there is an increased risk — albeit small — of suicide.
With respect to subtypes of dementia, older adults with Alzheimer disease were at higher risk of suicide, whereas those with vascular dementia were not at significantly higher risk of suicide than those without dementia. Alzheimer disease and vascular dementia share many clinical signs and symptoms. Both are characterized by cognitive decline, functional deterioration and neuropsychiatric symptoms that may present as behavioural alterations.45 However, some differences have been observed. Whereas memory and language function deficits prevail in patients with Alzheimer disease, executive frontal lobe cognitive functions (such as attention, planning and speed of mental processing) are more impaired in patients with vascular dementia.46 Motor function is not as highly affected by Alzheimer disease47,48 as it is by vascular dementia.49,50 It is possible that patients with Alzheimer disease who have a less impaired ability to plan and execute suicide are at higher risk for suicide death. In South Korean clinical settings, if specialists cannot clearly identify dementia, they tend to diagnose patients with other/unspecified dementia, which may include other mental disorders. It is difficult to elucidate the mechanisms that determine why older adults with other/unspecified dementia are at an increased risk for suicide, suggesting the need for further research.
Mental disorders are a major predictor of suicide,30 and dementia is strongly associated with mental health conditions. Approximately 25% of patients with dementia had at least 1 other mental disorder.26,51 Our findings showed that the suicide risk of patients with dementia and other mental disorders was higher than that of patients without other mental disorders, particularly older patients diagnosed with other mental disorders before their dementia diagnosis. A previous study found that older patients diagnosed with other mental disorders and dementia during hospitalization showed a higher suicide risk than those diagnosed with only dementia.28 However, the previous study could not elucidate the timing of diagnosis of the other mental disorders among patients with dementia. Our results implied that clinicians who treat patients with dementia need to pay more attention to those with dementia and histories of other mental disorders before diagnosis to reduce the risk of suicide death.
Among mental disorder subtypes, our findings showed that patients with dementia and schizophrenia, mood disorders, or anxiety and somatoform disorders had an increased risk of suicide death. A Taiwan cohort study reported that suicide posed the greatest risk of mortality in patients with schizophrenia.52 An epidemiologic survey out of the United States showed that patients with anxiety or depression were at increased risk of suicide.53 Our findings suggest that patients with dementia and schizophrenia, mood disorders, or anxiety or somatoform disorders require special focus.
Among patients with dementia, men and women, young-old adults, old-old adults and those with comorbidities all had an increased risk of suicide death compared to their counterparts without dementia. A previous study revealed that the presence of chronic comorbidities did not affect suicide risk among persons with dementia.28 This study used Charlson’s comorbidity index to examine coexisting chronic disorders. In contrast, we measured the presence of specific chronic diseases (diabetes mellitus, hypertension, dyslipidemia, Parkinson disease, stroke, ischemic heart disease, chronic kidney disease and cancer). Our results implied that a history of comorbidities before dementia diagnosis may increase the risk of suicide death.
Limitations
This study had several limitations. First, we could not determine dementia severity from the medical records. Future research is warranted to explore suicide risk over a specific period, considering dementia severity. Second, although education level,54 death of a child55 or spouse,56 living alone,57 marital status,58 migrant status59 and lifetime personal history of suicide attempts60 are risk factors for death by suicide, we could not consider these variables as covariates in this study because our database did not include this information. Finally, our study cohort consisted entirely of elderly South Korean people who demonstrate a higher suicide rate (53.3 per 100 000 population) than similar populations in the United States (14.3 per 100 000 population), the United Kingdom (7.0 per 100 000 population) and Japan (22.8 per 100 000 population). Therefore, caution needs to be exercised when generalizing our results to populations with dissimilar backgrounds (e.g., younger populations or people from countries with lower suicide rates than South Korea).
Conclusion
This is the first longitudinal retrospective cohort study to explore suicide risk within 1 year after a dementia diagnosis using nationally representative data. Our results indicated that patients with dementia had an increased risk of suicide death within 1 year after diagnosis compared to those without dementia, regardless of the presence of other mental disorders. Given the elevated suicide risk in the first year after a dementia diagnosis, early intervention for suicide prevention should be provided to older adults with dementia.
Acknowledgments
The authors thank Enago (enago{at}enago.co.kr) for English-language editing.
Footnotes
Competing interests: None declared.
Contributors: All authors designed the study. J. Choi and E. Han acquired the data, which all authors analyzed. All authors wrote and reviewed the article. All authors approved the final version to be published and can certify that no other individuals not listed as authors have made substantial contributions to the paper.
Funding: This work was supported by the National Research Foundation of Korea [grant number: 2019R1A2C1003259], the Yonsei University Research Fund (Post Doc. Researcher Supporting Program) of 2019 [2019-12-0129], and the National Research Foundation of Korea [grant number: 2020R1I1A1A01053104].
- Received December 23, 2019.
- Revision received June 26, 2020.
- Accepted July 10, 2020.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is non-commercial (i.e. research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/